
Lyme disease is a serious condition caused by six species of spirochetal bacteria, most commonly Borrelia burgdorferi in North America, following a deer tick bite that requires treatment. Clinical disease can occur within days to several months following a tick bite. Lyme disease is endemic to the northeastern states from Virginia to eastern Canada, the upper Midwest, particularly Wisconsin and
Minnesota, and northern California. The following provides key points regarding diagnosis, treatment, prophylaxis and tick removal.
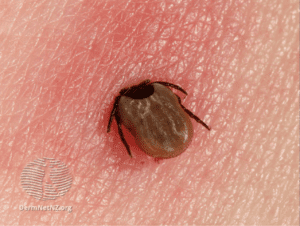
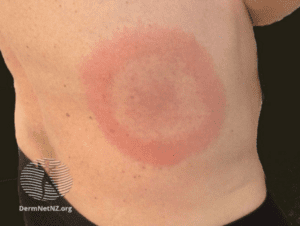
Ixodes tick and Erythema Migrans images courtesy DermNetNZ.org
Early disseminated disease features:
Note: The CDC has updated the Lyme laboratory screening algorithm
When cleared by FDA for this purpose, serologic assays that utilize a second EIA in place of western immunoblot assay are acceptable alternatives for the serologic diagnosis of Lyme disease
Note: When EM is present and patient has been to a Lyme endemic area serologic testing is not recommended and treatment can be initiated following clinical diagnosis
There is no convincing biologic evidence for the existence of symptomatic chronic B. burgdorferi infection among patients after receipt of recommended treatment regimens for Lyme disease. Antibiotic therapy has not proven to be useful and is not recommended for patients with chronic (⩾6 months) subjective symptoms after recommended treatment regimens for Lyme disease.
CDC: Lyme Disease Diagnosis, Treatment and Testing
Signs and Symptoms of Untreated Lyme Disease
Minnesota Department of Natural Resources: Deer Ticks
CDC: Lyme Disease Transmission
JAMA: Lyme Disease in 2018 – What Is New (and What Is Not)
FDA clears new indications for existing Lyme disease tests that may help streamline diagnoses
CDC: Updated CDC Recommendation for Serologic Diagnosis of Lyme Disease
BMJ State-of-the-Art Review: Lyme borreliosis: diagnosis and management
Please log in to ObGFirst to access this page