
Ventricular Septal Defect – Implications for the Fetus
WHAT IS IT?
- The left and right ventricles are connected through a “hole” in the wall/septum between the two chambers
- Most common cause of all congenital heart defects (CHDs), comprising 50% of all CHDs
- Estimated to occur in approximately 42/10,000 babies born
- Isolated VSD accounts for 20% of all birth defects
- Ventricular Septal Defects (VSDs) can be a single defect or multiple involving various components of the ventricular septum
- The ventricular septum is made up of two major morphological components, muscular and membranous, and these components are further divided depending on location relative to other heart structures
KEY POINTS:
- Cause of VSD is often unknown, but may be associated with common genetic issues such as Down syndrome (Trisomy 21) or 22q11.2 deletion syndrome, as well as more rare disorders
- Can range from small isolated finding that will close on its own, to complex CHD requiring surgical repair and interdisciplinary team management
- Consider genetic consultation and option for prenatal diagnostic testing to identify potential cause as may influence management
- ACOG guidance recommends offering invasive testing using microarray in the setting of fetal structural anomalies seen on prenatal ultrasound
- Further expert fetal imaging including fetal echocardiography is valuable to determine whether finding is isolated, as well as to determine prognosis and perinatal management plan
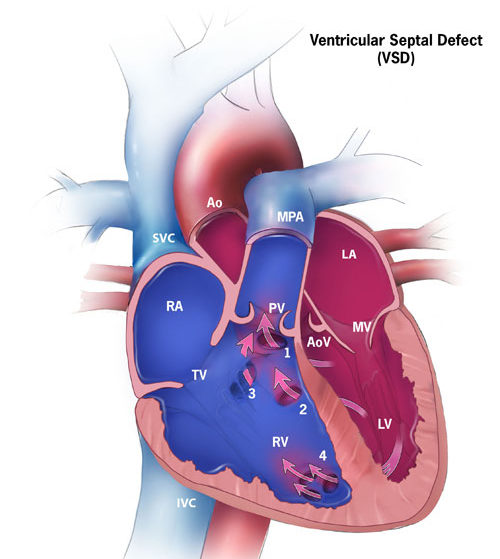
Image credit: Centers for Disease Control and Prevention, National Center on Birth Defects and Developmental Disabilities
Learn More – Primary Sources:
AHA Circulation Journal Review: Ventricular Septal Defects
CDC: Facts About Ventricular Septal Defect
Locate a genetic counselor or genetics services:
Genetic Services Locator-ACMG
Genetic Services Locator-NSGC
Genetic Services Locator-CAGC

Tetralogy of Fallot- A Critical Congenital Heart Defect
WHAT IS IT?
Tetralogy of Fallot (TOF) is a congenital heart defect, that occurs in approximately 1 in every 2,500 live births and accounts for 7-10% of all congenital heart defects
TOF is comprised of 4 major abnormalities:
- Pulmonary Infundibular Stenosis: narrowing of right ventricular outflow track
- Overriding aorta: the aortic valve is connected to both ventricles
- Ventricular Septal Defect: the left and right ventricles are connected through a “hole”
- Right Ventricular Hypertrophy: the right ventricular wall muscle is thicker than usual
Cause is usually unknown, but may be associated with genetic issues
- Consider 22q11.2 deletion syndrome and Down syndrome
- ACOG guidance recommends offering invasive testing using microarray in the setting of fetal structural anomalies seen on prenatal ultrasound
Categorized as a ‘critical congenital heart defect’, which means a likelihood of surgery and intensive management and procedures during the first year of life

Credit: Mariana Ruiz Villarreal
Learn More – Primary Sources:
CDC: Facts about Tetralogy of Fallot
CDC: Facts about Critical Congenital Heart Defects
CDC: Improved National Prevalence Estimates for 18 Selected Major Birth Defects
ISUOG Practice Guidelines (updated): sonographic screening examination of the fetal heart
ACOG Practice Bulletin No. 162: Prenatal Diagnostic Testing for Genetic Disorders
ACOG Committee Opinion No. 682: Microarrays and Next-Generation Sequencing Technology: The Use of Advanced Genetic Diagnostic Tools in Obstetrics and Gynecology

Understanding Transposition of the Great Arteries
WHAT IS IT?
In a normal heart, the pulmonary artery carries deoxygenated blood to the lungs. Oxygenated blood returns to the left side of the heart and the aorta then pumps the oxygenated blood to the rest of the body. In Transposition of the Great Arteries (TGA), the pulmonary artery and aorta have changed places (i.e., they are transposed). Therefore:
- The pulmonary artery, which usually arises from the right side of the heart and carries deoxygenated blood to the lungs, will now connect to the left side of the heart and send oxygenated blood back to the lungs
- The aorta, which usually arises from the left (oxygenated) side of the heart, is now exiting the right side and therefore will carry deoxygenated blood to the rest of the body, bypassing the lungs
- 5 out of 10,000 babies are born with TGA
- TGA is referred to as a ‘cyanotic’ (lacking oxygen) defect leading to babies with bluish discoloration and shortness of breath, with symptoms dependent on whether there is any ability for the deoxygenated and oxygenated blood to mix and be delivered to the rest of the body
- Surgery is often necessary shortly after birth, especially in the case of complete TGA (also known as d-TGA referring to ‘dextroposition’) which is considered a ‘critical congenital heart defect’
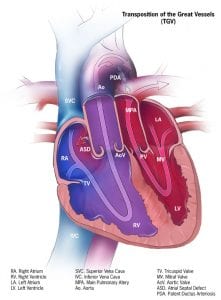
Image credit: Centers for Disease Control and Prevention, National Center on Birth Defects and Developmental Disabilities
KEY POINTS:
- While TGA can be diagnosed prenatally on ultrasound, it may not always be detected
- In the majority of cases, a cause is not readily apparent
- In some cases, TGA can be associated with genetic abnormalities and therefore, if a prenatal diagnosis is made or suspected, referral for genetic counseling is recommended, in addition to high risk obstetrical services, neonatology and pediatric cardiology
- TGA is sometimes referred to as Transposition of the Great Vessels (TGV)
Learn More – Primary Sources:
CDC: Facts about dextro-Transposition of the Great Arteries (d-TGA)
Circulation-AHA journal: Transposition of the Great Arteries
CDC: Facts about Critical Congenital Heart Defects
Current diagnosis and treatments for critical congenital heart defects
Fetal Growth and Neurodevelopmental Outcome in Congenital Heart Disease
Locate a Genetic Counselor or Genetics Services:
Genetic Services Locator-ACMG
Genetic Services Locator-NSGC
Genetic Services Locator-CAGC
Locate a Maternal Fetal Medicine Specialist:
Maternal Fetal Medicine Specialist Locator-SMFM

Atrial Septal Defect (ASD) – Summary and Implications
WHAT IS IT?
- Atrial septal defects can be generally classified into 3 subtypes:
- Ostium secundum ASD: defect of the atrial septum that involved the region of the fossa ovalis
- More common in females (65-75%)
- While endocardial cushion defects are more commonly associated with Down syndrome, secundum ASDs have also been associated with Down syndrome
- Ostium primum ASD: actually an atrioventricular (AV) septal defect, sometimes referred to as an AV canal defect or endocardial cushion defect
- Associated with Down syndrome (15 to 20%) but may also be associated with other chromosomal abnormalities such as DiGeorge syndrome (22q11 deletion syndrome)
- Sinus venosus ASD: occurs at the junction of the right atrium and superior vena cava and is almost always associated with partial anomalous pulmonary venous return
- May be associated with arrhythmias
- Other uncommon subtypes do exist
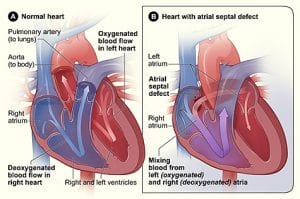
Image credit – National Heart Lung and Blood Institute (NIH)
CAUSE:
ASD is typically sporadic, however may occur as an isolated finding in families or as part of various genetic syndromes including but not limited to Down syndrome, DiGeorge syndrome and Holt-Oram syndrome which involves variable radial ray anomalies.
KEY POINTS:
- Can range from small isolated finding that will close on its own, to complex congenital heart defect (CHD) requiring surgical repair and interdisciplinary team management
- Consider genetic consultation to identify potential cause as may influence management
- ACOG guidance recommends offering invasive testing using microarray in the setting of fetal structural anomalies seen on prenatal ultrasound
Learn More – Primary Sources:
AHA Circulation Journal -Atrial Septal Defects in the Adult
CDC: Facts about Atrial Septal Defect
ACOG Practice Bulletin No. 162: Prenatal Diagnostic Testing for Genetic Disorders
Locate a Genetic Counselor or Genetics services:
Genetic Services Locator-ACMG
Genetic Services Locator-NSGC
Genetic Services Locator-CAGC







