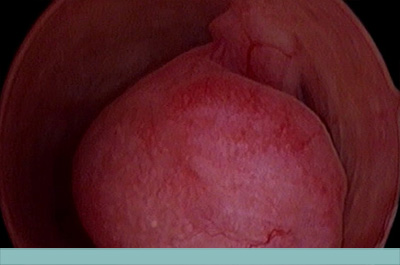
Endometrial Polyps
BACKGROUND:
Endometrial polyps are a common condition that may be associated with abnormal uterine bleeding, infertility, and pre-malignant and malignant conditions. Reported prevalence ranges between 7.8 to 32.9%, depending on diagnostic method and population studied (Salim, Dreisler, Fabres). Prevalence tends to increase with age and has been reported more with post menopausal (12%) than premenopausal women (6%) (Salim).
An endometrial polyp is defined as a localized hyperplastic overgrowth of endometrial glands and stroma that projects from the endometrial surface (Kim). They may be single, multiple, sessile, or pedunculated. The exact cause is unknown, however identified risk factors include: age, HTN, obesity, tamoxifen use (Salim). Both estrogen and progesterone regulate the balance of proliferation and apoptosis in the endometrium, and therefore appear to contribute to growth of polyps. However there have also been studies that show that women’s age and menopausal status do not significantly affect growth rate of polyps, suggesting that not all polyps are necessarily hormone dependent (Wong).
Roughly 44% of polyps in women are asymptomatic, therefore incidental findings are very common (Hassa). Abnormal uterine bleeding, including intermenstrual bleeding and post menopausal bleeding, is the most common symptom, occurring in 68% of women with polyps and (Salim, Golan). However, studies have also shown that symptomatology does not consistently correlate with polyp number, diameter, or site (Salim, Hassa). A recent study of 112 women managed for a mean of 22.5 months shows that there is no association between development on symptoms and polyp growth rate, so routine ultrasound to monitor growth cannot necessarily predict the onset of symptoms. This finding supports the rationale to encourage women with asymptomatic polyps to report symptoms rather than undergo routine U/S scans to monitor growth.The same study found that only 6.3 percent of polyps spontaneously regressed and that no identifiable factors were reliably associated with polyp growth and regression (Wong).
DIAGNOSIS:
TVUS is the first line imaging study of choice to evaluate women with abnormal bleeding. The best time to evaluate women with TVUS is day 10 of a woman’s cycle when endometrium is the thinnest. For those patients for whom U/S findings are inconclusive, postmenopausal women, or those who are candidates for expectant management, a diagnostic hysteroscopy or saline infused sonohysterogram are suggested as both are able to give a better indication of the presence and shape of the lesion of question.
Diagnosis can only definitively be made with histologic examination after specimen has been removed. Hysteroscopic polypectomy is the gold standard when it comes to removal of polyps as it carries a relatively low risk, and enables removal of the entire lesion in question under direct visualization (Salim).
MALIGNANT POTENTIAL:
Approximately 95% of polyps are benign (Baiocchi). The prevalence of malignant lesions among post menopausal women with polyps ranges in literature between 3-6%. A retrospective study by Bel at al identified risk factors associated with malignant polyps. These risk factors include: age, BMI, hormone replacement therapy, first degree episodes of GYN cancer in their family hx. This study concluded that the risk of malignancy is highest (12.3%) in patients at least 59 years old with abnormal uterine bleeding. The risk among other subgroups varied between 2.31-3.78%. Clinically, therefore, hysteroscopy should be performed with menopausal patients over 59 yo with endometrial polyp and postmenopausal bleeding (Bel).
There has been conflicting evidence regarding the size of polyp and its association with malignancy. Some studies report that polyps >1.5 cm in diameter are associated with an increased risk of malignancy. However a systematic review found that data was inconclusive with regard to polyp size and malignancy potential. (Baiocchi)
MANAGEMENT:
Hysteroscopic polypectomy is the gold standard in terms of removal of polyps. It provides safe and effective management that enables histologic assessment and direct visualization. Blind curettage may miss small polyps or structural abnormalities and is therefore not recommended.
Symptom free premenopausal women with polyps <10mm may be managed conservatively as long as they don’t have other risk factors for endometrial hyperplasia or cancer. In patients with infertility, removal has been shown to improve subsequent pregnancy (Bosteels). In post-menopausal women with endometrial polyps we recommend hysteroscopic polypectomy, as they carry the highest risk of malignancy. However, asymptomatic postmenopausal polyps, specially is smaller than 10mm, are unlikely to be malignant and observation is an option after counseling. A blind biopsy should never be used as a reliable means of polyp removal, as there is no way to know whether the entire lesion was removed. Even if an EMB yields histologically diagnosed polyp, this should be followed with hysteroscopy to ensure adequate removal.
KEY POINTS:
- Endometrial polyps are a common gynecologic disease that increases with age!
- Although the grand majority of polyps are benign, they do carry risk of malignancy
- Symptomatic polyps should be removed in all women
- Management of asymptomatic polyps depends on likelihood of malignancy associated with polyp or concerns of infertility
- Polyps should always be removed in post menopausal women, as they carry the greatest risk of malignancy
- Hysteroscopic polypectomy is the gold standard management option for polyp removal; and blind methods should be avoided when visual techniques are available
- Conservative treatments should be favored over radical treatments
Authors
Douglas B Timmons Jr MD MPH
Ashley K Ulker MD
Jose Carugno MD FACOG
Author Affiliation: Minimally Invasive Gynecologic Surgery at Miller School of Medicine
Learn More – Primary Sources:
Baiocchi et al., Malignancy in endometrial polyps: a 12-year experience
Bel et al., Risk of malignancy on suspicion of polyps in menopausal women
Hassa et al., Are the site, diameter and number of endometrial polyps related with symptomatology?
Salim et al., Diagnosis and management of endometrial polyps: a critical review of the literature
Wong et al., The natural history of endometrial polyps
Want to Read More About Office Hysteroscopy?
You can find the entire set of newsletters (in multiple languages) at the Hysteroscopy Newsletter Website.
Want to Learn More About Office Hysteroscopy with Colleagues from All Over the World?
Set aside time in your calendar now for the Global Congress on Hysteroscopy Barcelona, 30 April-3 May, 2019. With parallel tracks for everyone – beginners, advanced and expert. The Board of the Global Congress on Hysteroscopy includes representatives of ALL international endoscopy societies (ESGE, AAGL, ISGE, APAGE and MESGE) together with a group of relevant and independent hysteroscopists. It’s all about learning with each other, from each other.
Want to be notified about upcoming Hysteroscopy Newsletter posts here at The ObG Project?
All content in this entry was prepared by the above-named author(s) who retain full responsibility for content. The opinions expressed in this article are the author’s own and not those of The ObG Project. Links to third party websites are provided only as a convenience. The ObG Project does not review, control, or examine them. Therefore, The ObG Project is not responsible for the information, advertising, products, resources or other materials of any linked site or any link contained in a linked site. The inclusion of a link does not imply endorsement by the provider. In addition, please be aware that your use of any linked site is subject to the terms and conditions applicable to that site. Please direct any questions regarding linked sites to the webmaster of that site.
Are you an
ObG Insider?
Get specially curated clinical summaries delivered to your inbox every week for free